Patient assessment training utilizes realistic scenarios‚ aligning with National Registry skill sheets and mirroring common emergency calls‚ as detailed in resources from 1995 to 2025.
Importance of Scenario-Based Training

Scenario-based training is crucial for EMS providers‚ bridging the gap between theoretical knowledge and real-world application. Resources like the “Real-World EMT Scenarios Workbook (2024-2025)” emphasize critical thinking through 100 actual cases‚ covering airway‚ cardiology‚ trauma‚ and medical emergencies.
This approach allows for the development of clinical judgment‚ decision-making skills‚ and effective communication – all vital in dynamic emergency situations. Practicing with cases based on genuine emergency calls‚ as found in the “Patient Assessment Practice Scenarios” textbook (2011)‚ prepares providers for the unpredictable nature of the field.
Furthermore‚ it reinforces adherence to National Registry skill sheets‚ ensuring competency and readiness for certification. Ultimately‚ scenario training enhances patient care and improves outcomes.
National Registry Skill Sheet Alignment
Effective patient assessment training must directly correlate with the National Registry of Emergency Medical Technicians (NREMT) skill sheets. The “Patient Assessment Practice Scenarios” textbook (2011) is specifically designed to follow these guidelines‚ ensuring comprehensive coverage of required competencies.
This alignment is vital for successful certification and licensure. Scenarios should incorporate elements assessed during practical exams‚ such as accurate vital sign measurement (pulse‚ blood pressure‚ respiratory rate)‚ thorough patient history gathering (SAMPLE/OPQRST)‚ and appropriate scene assessment.
Resources emphasize the importance of demonstrating proficiency in these skills within realistic contexts‚ preparing candidates for the demands of the NREMT examination and real-world practice.
Real-World Emergency Call Relevance
Practical EMS training thrives on scenarios mirroring actual emergency calls. Resources like the “Real-World EMT Scenarios” workbook (2024-2025) provide 100 authentic cases‚ covering airway management‚ cardiology‚ trauma‚ medical emergencies‚ and operational challenges. These scenarios aren’t theoretical; they’re based on the types of incidents EMTs frequently encounter.
Examples include assessing a seizure patient (postictal state‚ SAMPLE history) or an intoxicated individual (neurological assessment‚ SpO2 evaluation). The goal is to bridge the gap between textbook knowledge and practical application‚ fostering critical thinking and sound clinical judgment.
This approach prepares providers to confidently handle diverse and unpredictable real-world situations.

Core Components of Patient Assessment
Effective assessment involves initial impressions‚ scene safety‚ the ABCDE primary survey‚ vital signs‚ and detailed history gathering – crucial elements for proper patient care.
Initial Impression & Scene Safety
Forming an initial impression is paramount upon arrival‚ quickly assessing the overall situation and number of patients. Simultaneously‚ ensuring scene safety is non-negotiable – protecting yourself‚ your team‚ and the patient from further harm. This includes identifying potential hazards like traffic‚ unstable structures‚ or hazardous materials.
A rapid scan of the surroundings provides vital clues about what may have occurred. Observing the patient’s position‚ apparent age‚ and level of distress contributes to a preliminary understanding. Maintaining body substance isolation (BSI) is essential from the outset. The 1995 EMT-I scenarios emphasize rapid trauma assessment and hemorrhage control‚ highlighting the need for preparedness. Prioritizing safety allows for a focused and effective patient assessment‚ setting the stage for appropriate interventions.

Primary Assessment – ABCDE
The ABCDE mnemonic guides the systematic primary assessment: Airway‚ Breathing‚ Circulation‚ Disability‚ and Exposure. First‚ ensure a patent airway – look‚ listen‚ and feel for obstructions. Next‚ assess breathing – rate‚ depth‚ and quality. Simultaneously‚ evaluate circulation by checking pulse and skin condition; a pulse of 120 was noted in one scenario.
Disability refers to a quick neurological assessment‚ noting the patient’s level of consciousness (oriented to person only in one case). Finally‚ Exposure involves briefly exposing the patient to identify any hidden injuries. Throughout‚ continuous monitoring of vital signs is crucial. Resources from 2024-2025 emphasize critical thinking within these steps‚ preparing EMTs for real-world challenges.
Vital Signs Measurement
Accurate vital signs are fundamental to patient assessment. Pulse assessment reveals rate and quality – one scenario documented a pulse of 120. Blood pressure measurement provides insight into circulatory status‚ with a reading of 110/ noted in a case study. Respiratory rate and quality are crucial; shallow breathing at 24 breaths per minute was observed.
Pupil examination assesses neurological function – pupils were described as PERRL (Pupils Equal‚ Round‚ Reactive to Light) and slow to react in one instance. Blood Glucose Level (BGL) monitoring is essential‚ registering at 120 and 85 in different scenarios; Consistent documentation‚ as emphasized in training materials from 2011 and beyond‚ is paramount.
Pulse Assessment
Pulse assessment is a cornerstone of vital signs evaluation‚ providing critical information about cardiovascular function. Determining the pulse rate‚ rhythm‚ and quality is essential for identifying potential issues. A scenario details a pulse rate of 120 beats per minute in an intoxicated patient‚ indicating possible tachycardia.
Assessing pulse strength – whether bounding‚ strong‚ weak‚ or thready – offers further diagnostic clues. Documentation should include the location where the pulse was assessed (radial‚ carotid‚ etc.); Training resources from 2011 and updated workbooks emphasize consistent pulse assessment as a key skill for EMTs‚ crucial for accurate patient evaluation and informed decision-making in emergency situations.
Blood Pressure Measurement
Blood pressure measurement is a vital component of patient assessment‚ reflecting the force of blood against artery walls. Accurate measurement requires proper technique and equipment – a cuff of appropriate size and a stethoscope. A scenario presented indicates a blood pressure of 110/– in an intoxicated 18-year-old female‚ highlighting the importance of complete documentation.
Understanding systolic and diastolic pressures is crucial for interpreting results. Training materials‚ spanning from 1995 to 2025‚ consistently emphasize blood pressure as a key indicator of perfusion and overall patient status. Variations from normal ranges can signal shock‚ hemorrhage‚ or other critical conditions‚ guiding immediate interventions and transport decisions.
Respiratory Rate & Quality
Assessing respiratory rate and quality is paramount in patient evaluation‚ revealing the effectiveness of oxygenation and ventilation. A presented scenario details an intoxicated patient exhibiting a respiratory rate of 24 breaths per minute‚ described as shallow. This observation immediately raises concern for potential hypoventilation and inadequate oxygen delivery.
Training resources‚ dating from 1995 through 2025‚ consistently stress the need to observe chest rise and fall‚ noting any signs of labored breathing‚ accessory muscle use‚ or abnormal sounds. Accurate assessment informs decisions regarding supplemental oxygen administration‚ airway management‚ and the urgency of transport‚ ensuring optimal patient outcomes in diverse emergency situations.
Pupil Examination
Pupil assessment provides crucial neurological insights during patient evaluation. Scenario documentation highlights findings of “perrl” – pupils equal‚ round‚ reactive to light – in an intoxicated 18-year-old female. However‚ another scenario notes pupils being “slow to react” in a postictal patient‚ indicating potential altered mental status or neurological compromise.
Comprehensive training‚ spanning resources from 1995 to 2025‚ emphasizes evaluating pupil size‚ symmetry‚ and reactivity to light. Abnormalities can signal head injury‚ drug overdose‚ or other critical conditions. Accurate documentation and interpretation are vital for guiding treatment decisions and informing ALS/transport considerations‚ ensuring appropriate care based on neurological findings.
Blood Glucose Level (BGL) Monitoring
Blood Glucose Level (BGL) assessment is a critical component of patient evaluation‚ particularly in altered mental status cases. Documentation from scenarios reveals a BGL of 120 in a postictal patient‚ considered within the normal range‚ yet doesn’t exclude other underlying causes for their condition. Conversely‚ an intoxicated patient presented with a BGL of 85‚ also within normal limits‚ but requiring consideration alongside other clinical findings.
Training materials from 1995-2025 emphasize BGL monitoring to rule out hypoglycemia as a cause of altered mental status or neurological deficits. Prompt identification and treatment of low blood sugar can significantly impact patient outcomes‚ highlighting the importance of this quick and readily available assessment tool during emergency response.
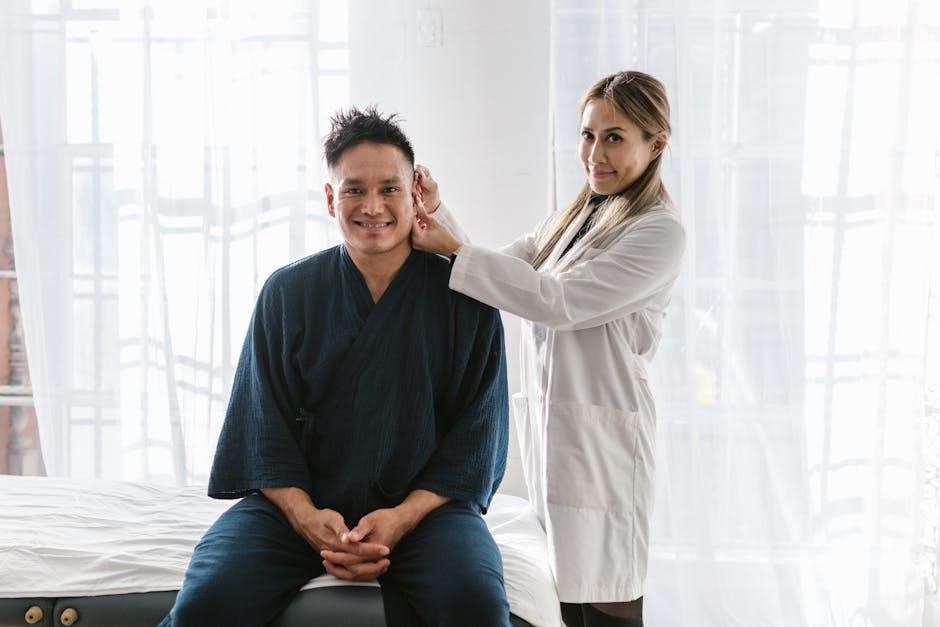
Common Patient Assessment Scenarios
Realistic scenarios include seizure patients (postictal states‚ SAMPLE history)‚ intoxicated individuals (neurological & skin assessments)‚ and those in respiratory distress requiring rapid trauma assessments.
Seizure Patient Assessment
Assessing a seizure patient demands a systematic approach‚ beginning with scene safety and a focused evaluation of the postictal state. Documentation should reflect pupil reactivity – noting if they are equal and slow to react – alongside a blood glucose level‚ ideally around 120.
Crucially‚ gather a detailed SAMPLE history: specifically inquiring about prior seizure history‚ duration of the event (like the reported four minutes)‚ and time since cessation (five minutes prior to EMS arrival).
Pain assessment is vital‚ but often absent in postictal patients‚ who may present primarily with lethargy. Confirm allergies‚ medications‚ and family history. Based on assessment‚ ALS intercept and transport are often indicated‚ alongside continuous airway monitoring and supplemental oxygen administration as needed.
Postictal State Evaluation
Evaluating the postictal state requires careful neurological assessment. Observe for altered mental status‚ often manifesting as confusion or lethargy‚ as seen in patients post-seizure. Document pupil response – noting if equal and slow to react – as this can indicate neurological involvement.
A focused assessment should also include checking blood glucose levels; a reading of 120 is within normal limits‚ but fluctuations should be investigated.
Determine the seizure duration and time since termination‚ crucial for understanding the patient’s recovery phase. Assess for any signs of injury sustained during the seizure. Thorough documentation of these findings guides subsequent treatment and transport decisions.
SAMPLE History Gathering (Seizure Scenario)
Employing the SAMPLE mnemonic is vital when gathering history from a seizure patient or bystanders. Signs and Symptoms: note the seizure type and duration (4 minutes in one case). Allergies: confirm any known allergies (none reported).
Medications: ascertain current medications (none reported). Past medical history: inquire about prior seizure activity (none reported). Last oral intake: determine when the patient last ate or drank.
Events leading up to the seizure: understand the circumstances preceding the event. This detailed history‚ combined with physical assessment findings‚ informs appropriate ALS consideration and transport decisions.
ALS/Transport Considerations (Seizure)
Following seizure assessment‚ ALS intercept may be crucial‚ particularly with prolonged or repeated events. Monitor airway patency and administer supplemental oxygen if indicated‚ addressing potential hypoxia. Transport is generally warranted for postictal patients‚ even if the seizure has ceased‚ for further evaluation.
Consider the postictal state – lethargy requires careful monitoring during transport. Communicate assessment findings clearly to receiving facilities‚ including seizure duration and any associated injuries.
Document all interventions and the patient’s response. Continuous reassessment of ABCs is paramount throughout transport‚ ensuring patient stability until arrival at the hospital.
Intoxicated Patient Assessment
Assessing intoxicated patients requires a systematic approach‚ acknowledging altered mental status. Neurological assessment is key – evaluate orientation to person‚ place‚ and time‚ noting any deficits. Observe for signs of trauma masked by intoxication‚ as altered perception increases risk. Skin assessment reveals clammy skin‚ while SpO2 monitoring is vital‚ aiming for adequate oxygenation.
A focused SAMPLE history is crucial‚ despite potential unreliability. Vital signs‚ like pulse (120 bpm) and blood pressure (110/–)‚ provide baseline data. Be mindful of respiratory rate (24‚ shallow) and potential compromise.
Neurological Assessment (Intoxication)
Neurological evaluation in intoxicated patients focuses on level of consciousness and responsiveness. Assess orientation to person‚ place‚ time‚ and event – deficits are common. Note any slurred speech‚ incoordination‚ or altered gait. Pupil examination should reveal PERRL (Pupils Equal‚ Round‚ Reactive to Light)‚ though intoxication can sometimes affect reactivity.
Glasgow Coma Scale (GCS) can be utilized‚ but interpretation requires caution due to substance effects. Look for signs of head injury‚ even if the patient denies trauma. Document any observed neurological abnormalities objectively‚ recognizing potential unreliability of patient reporting.
Skin & SpO2 Evaluation (Intoxication)
Skin assessment in intoxicated patients should include color‚ temperature‚ and moisture. Clammy skin‚ as observed in one scenario‚ can indicate dehydration or underlying medical issues. Evaluate capillary refill time‚ though it may be unreliable if perfusion is compromised. Pulse oximetry (SpO2) is crucial; a reading of 91% in a case study suggests potential respiratory compromise.
Low SpO2 warrants supplemental oxygen administration. Assess for cyanosis around the lips and nail beds. Remember that alcohol and other substances can depress respiratory drive‚ leading to hypoxemia. Continuously monitor SpO2 and document any changes‚ correlating them with the patient’s clinical presentation.
SAMPLE History Gathering (Intoxication)
Signs and Symptoms: Document the patient’s level of consciousness‚ orientation (person‚ place‚ time‚ event – noting deficits as seen in a scenario)‚ and any reported complaints. Observe for slurred speech or incoordination. Allergies: Specifically inquire about any known allergies‚ including reactions to medications or substances.
Medications: Obtain a list of current medications‚ including over-the-counter drugs. Past medical history: Ask about pre-existing conditions. Last oral intake: Determine when and what the patient last ate or drank. Events leading up to the incident: Crucially‚ ascertain what substance(s) were ingested and the quantity.
Respiratory Distress Patient Assessment
Initial assessment focuses on identifying the severity of respiratory compromise. A rapid trauma assessment is crucial to rule out underlying injuries contributing to distress. Prioritize airway management‚ ensuring patency and considering adjuncts if needed. Simultaneously‚ assess for and control any visible hemorrhage‚ as blood loss can exacerbate respiratory issues.
Observe respiratory effort – noting rate‚ depth‚ and use of accessory muscles. Auscultate lung sounds for wheezes‚ crackles‚ or diminished breath sounds. Administer supplemental oxygen and prepare for potential assisted ventilation. Continuous monitoring of vital signs is paramount throughout the assessment and intervention process.
Rapid Trauma Assessment
The rapid trauma assessment is a systematic‚ head-to-toe evaluation performed to identify life-threatening injuries. Students must develop rapport with the patient while swiftly assessing for obvious deformities‚ abrasions‚ contusions‚ and tenderness (DCAP-BTLS). Maintaining body substance isolation is essential throughout the process.
Palpate the skull‚ face‚ and cervical spine‚ assessing for stability. Auscultate the chest for breath sounds and palpate for flail segments. Evaluate the abdomen for distension‚ guarding‚ and rebound tenderness. Inspect and palpate extremities for fractures and neurovascular compromise.
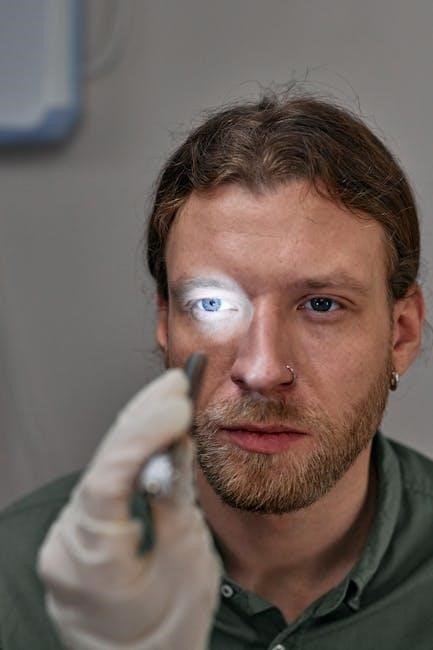
Hemorrhage Control
Effective hemorrhage control is paramount in trauma care‚ directly impacting patient outcomes. Students should practice techniques to swiftly stop bleeding while adhering to strict body substance isolation protocols. Direct pressure remains the initial intervention‚ applied firmly to the wound site using a sterile dressing.
Elevation of the injured extremity‚ when feasible‚ assists in reducing blood flow. Tourniquets are utilized for severe‚ life-threatening extremity hemorrhage when direct pressure fails. Proper tourniquet application and documentation are crucial. Ongoing assessment for distal pulses and skin perfusion is vital post-tourniquet placement.
Airway Management Techniques
Maintaining a patent airway is fundamental in emergency medical care‚ especially for patients in respiratory distress. Initial assessment focuses on identifying airway obstruction – look‚ listen‚ and feel for breathing. Basic techniques include the head-tilt/chin-lift maneuver‚ cautiously applied unless spinal injury is suspected.
Jaw-thrust maneuver is preferred in potential cervical spine trauma. Supplemental oxygen administration is crucial‚ utilizing nasal cannula or non-rebreather masks. Oropharyngeal and nasopharyngeal airways may assist in maintaining airway patency. Continuous monitoring of respiratory rate‚ depth‚ and oxygen saturation is essential throughout assessment and intervention.
Advanced Assessment Techniques
Detailed patient history‚ utilizing SAMPLE and OPQRST‚ alongside thorough trauma assessment focusing on mechanism of injury‚ refines initial findings for accurate diagnosis.
SAMPLE History – Detailed Questionnaire
Signs and Symptoms: Carefully document the patient’s reported complaints and observed conditions‚ noting specifics like seizure duration (4 minutes‚ as in one scenario) and altered mental status. Allergies: Confirm any known allergies to medications or environmental factors. Medications: Obtain a complete list of current medications‚ if available‚ crucial for understanding potential interactions.
Past medical history: Investigate pre-existing conditions‚ such as a history of seizures (or lack thereof‚ as noted in a scenario)‚ and relevant family history. Last oral intake: Determine when the patient last ate or drank anything‚ important for potential gastrointestinal issues or aspiration risk. Events leading up to the incident: Gather a detailed account of the events preceding the emergency‚ including the circumstances surrounding a seizure or intoxication.
This comprehensive approach‚ as emphasized in training materials from 1995-2025‚ ensures thorough data collection.
OPQRST Pain Assessment
Onset: Determine when the pain began and if it was sudden or gradual. Provocation/Palliation: Identify factors that worsen or relieve the pain – for example‚ movement or rest. Quality: Ask the patient to describe the pain (sharp‚ dull‚ crushing‚ etc;). Region/Radiation: Pinpoint the location of the pain and if it radiates to other areas.
Severity: Utilize a pain scale (0-10) to quantify the pain level. Time: Explore the pain’s duration – is it constant‚ intermittent‚ or fluctuating? In scenarios‚ note if “no pain” is reported‚ like in the postictal state following a seizure.
This systematic evaluation‚ highlighted in resources spanning 1995-2025‚ aids in accurate pain assessment and appropriate intervention‚ crucial for effective EMS care.
Trauma Assessment – Mechanism of Injury
Mechanism of Injury (MOI) is crucial in trauma assessment‚ helping predict potential internal injuries. Consider factors like vehicle speed‚ intrusion into the vehicle‚ ejection‚ and pedestrian impact. High-energy mechanisms – falls from significant heights or penetrating trauma – demand a thorough rapid trauma assessment‚ focusing on hemorrhage control.
Resources from 1995 emphasize student development of rapport while performing this assessment. Prioritize identifying life-threatening conditions.
Understanding the forces involved guides the assessment‚ informing the need for ALS intervention and transport‚ as detailed in training materials from 1995 to 2025.

Resources & Further Learning
Comprehensive resources include textbooks (2011)‚ workbooks (2024-2025)‚ and older training scenarios (1995) to enhance patient assessment skills and critical thinking.
Patient Assessment Practice Scenarios Textbook (2011)
This 2011 textbook serves as a foundational resource for mastering patient assessment techniques. It meticulously follows the National Registry skill sheets‚ ensuring alignment with certification standards and providing a structured learning path for aspiring EMS professionals. The book distinguishes itself by basing its cases on real-world emergency calls‚ offering practical relevance and preparing providers for the diverse challenges encountered in the field.
With a substantial 610 pages‚ the textbook delivers comprehensive coverage of essential concepts and procedures. It focuses on developing proficiency in both assessment and management of patients‚ equipping learners with the skills needed to effectively handle a wide range of medical emergencies. This resource is invaluable for students and practitioners seeking to refine their clinical judgment and enhance patient care.
Real-World EMT Scenarios Workbook (2024-2025)
This workbook‚ updated for 2024-2025‚ provides an intensive critical thinking experience through 100 actual scenarios. Each scenario is accompanied by 700 critical thinking questions‚ designed to challenge EMTs and enhance their decision-making abilities in high-pressure situations. The content comprehensively covers vital areas including Airway management‚ Cardiology‚ Trauma‚ Medical emergencies‚ and EMS Operations.
Unlike traditional textbooks‚ this resource emphasizes practical application and problem-solving. It forces users to analyze complex situations‚ prioritize interventions‚ and justify their actions – skills essential for success in the field. This workbook is an excellent supplement to formal training‚ offering a dynamic and engaging way to solidify understanding and prepare for real-world challenges.
Emergency Medical Technician-I Training Scenarios (1995)
Published in 1995‚ these scenarios focus on developing crucial patient interaction and rapid assessment skills. Students are expected to establish rapport with patients while performing a swift trauma assessment‚ prioritizing life-threatening conditions. A key component involves hemorrhage control‚ always maintaining strict body substance isolation protocols.
Essential equipment for these exercises includes a blood pressure cuff‚ stethoscope‚ penlight‚ patient care report (run sheet)‚ and a fully stocked trauma kit. Scenarios are designed to simulate real-world emergencies‚ requiring students to apply their knowledge and skills under pressure. The goal is to prepare EMT-I candidates for effective patient care and safe operational practices.